Alpha-1 Antitrypsin Deficiency (Alpha-1) can cause panniculitis, an uncommon skin condition. Panniculitis causes painful, raised red bumps to form on the skin. Treatment can help manage this condition.
What is panniculitis?
Panniculitis is an uncommon skin condition. It can be caused by several conditions, including Alpha-1. Panniculitis is rare in people with Alpha-1.
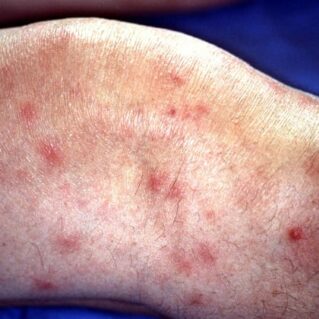
Panniculitis causes raised — sometimes painful — red bumps to form on the skin. These bumps may break open and leak an oily fluid. Panniculitis sometimes turns into deep ulcers in the skin where the tissue breaks down. These spots can be painful to the touch. The medical term for this is “necrotizing panniculitis.”
How does Alpha-1 cause panniculitis?
People with Alpha-1 do not have enough alpha-1 antitrypsin (AAT). Without AAT, the fatty tissue under the skin (called the panniculus) weakens and breaks down. This causes panniculitis.
Where do people get panniculitis?
Panniculitis can appear anywhere on the body but most often appears on the thighs, buttocks, and other parts of the body that are under pressure.
When do people get panniculitis?
Panniculitis spots sometimes develop after some kind of trauma or injury to the skin that would be minor in most people, such as vigorous exercise, intravenous injections, or cryosurgery (surgery that involves freezing the skin).
Panniculitis occurs equally among men and women, usually developing at an average age of 40.
How is panniculitis treated?
People with Alpha-1 who have panniculitis are sometimes treated with augmentation therapy. Augmentation therapy raises the levels of the AAT protein in the body using AAT protein taken from the blood of healthy donors.
Unfortunately, panniculitis caused by Alpha-1 does not improve with antibiotics or steroids as it does in people without Alpha-1.
New therapies for Alpha-1 and its complications are an expanding area of research. Treatment options for panniculitis will improve as this research matures.
If you have Alpha-1 and develop signs and symptoms of panniculitis, talk to your doctor about treatment options











